EDS Awareness Month

What is EDS?
The Ehlers-Danlos syndromes (EDS) are a group inherited connective tissue disorders caused by genetic changes that affect connective tissue. Each type of EDS has its own features with distinct diagnostic criteria. Some characteristics are seen across all types of EDS, including joint hypermobility, and tissue fragility.
What is HSD?
Hypermobility spectrum disorders (HSD) are connective tissue disorders that cause joint hypermobility, instability, and injury.
Both EDS and HSD.
Both conditions can cause pain and other problems such as fatigue, headaches, GI problems, and autonomic dysfunction.
Non-Visible Disability: What you see, What you don’t

If you see someone using mobility aids, it is easy to recognize a visible impairment or disability. But it is not always possible to know if someone has a non-visible disability, because not all disabilities can be instantly seen or are obvious to others.
Some people with disabilities that are not obvious prefer the phrase ‘non-visible disability’. This is because the word ‘invisible’ can imply the disability does not exist. ‘Hidden’ disability can imply a person is hiding their disability on purpose.
EDS and HSD and chronic conditions may affect many areas of the body, some of which are visible and some are not. Having a non-visible disability can affect someone’s life as much as a visible disability. In fact, repeated experience with stigmatization and lack of support can create additional difficulties for a person with a non-visible disability.
A person with a non-visible disability such as EDS or HSD may need mobility aids all the time, part-time or intermittently, depending on their symptoms. Their symptoms may fluctuate in severity so that on some days, they require more support, rest, or mobility aids than on other days. It is common for people with non-visible disabilities to have limited energy or physical resilience. They may walk or function normally, until they cannot. In this circumstance, they use assistive devices to ration their mobility and functionality. This is why you may see someone with a non-visible disability socializing, at work, or at school, and you may not see symptoms of EDS or HSD. You often do not see the days with fatigue, pain, and other symptoms.
The iceberg image is a wonderful reminder that we are all more than what we appear to be on the surface.
Sources:
http://www.ehlers-danlos.com/
http://www.facebook.com/ehlers.danlos
disabilityunit.blog.gov.uk/2020/12/17/living-with-non-visible-disabilities/
Tips for Dealing with Coat Hanger Pain
Natalie Dowty, PT, MPT, EdD
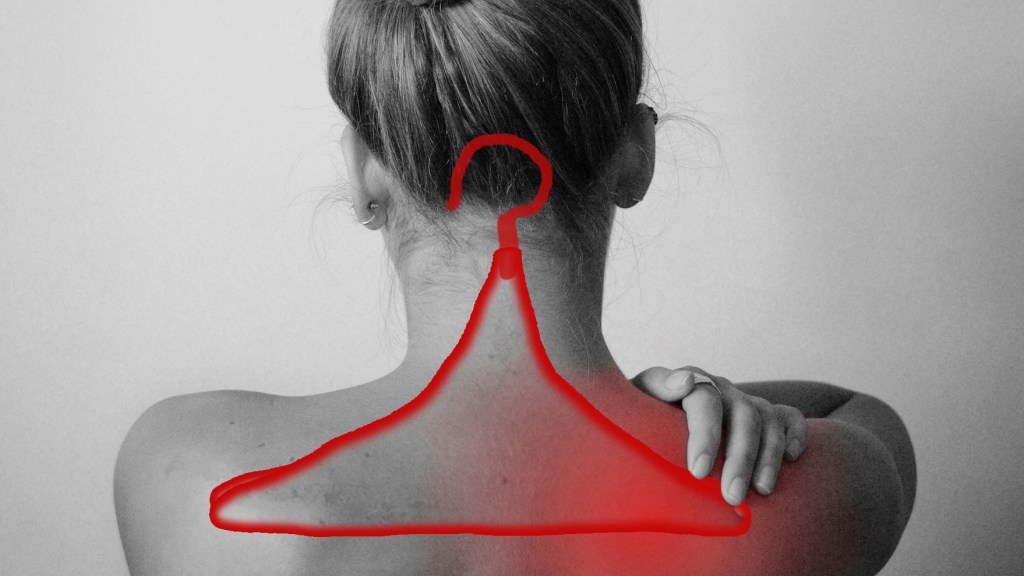
Coat hanger pain is seen in 93% of patients with dysautonomia and in 51% of patients with multiple system atrophy. It is one of the many “invisible” symptoms seen in people with dysautonomia and / or Ehlers Danlos Syndrome. This pain is often misdiagnosed as a spinal problem or fibromyalgia. However, the caused is thought to be poor blood flow in the muscles of the upper back and neck brought on by muscle imbalance and autonomic malfunction. The autonomic nervous system controls blood flow throughout the body, and when it’s not working properly, blood flow patterns can be disrupted. Postural dysfunction may have a role in exacerbation.
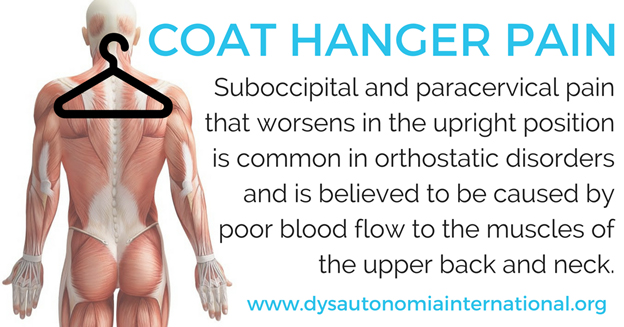
If you think you have Coat Hanger Pain, it’s a good idea to talk to your doctor.
At Integrative Wellness, Inc. Physical Therapy, we have been helping people manage Coat Hanger Pain and other related issues successfully for more than 20 years. We are here to help. Call 402-212-7444 to set up a consult.
Meanwhile, here are some tips that you can use right now to manage Coat Hanger Pain:
Positional release or postural time out.
1. This strategy is temporary relief from gravity. Before the pain gets bad, lay on your back, or in a horizontal position that is comfortably supported, with your knees up for five minutes or so. Doing this regularly on a schedule is especially helpful: for example, once an hour, or a mid-morning and mid-afternoon break. Positional release gives your posture muscles and autonomic nervous system a break from the stress of gravity. It allows your muscles to relax, and allows more normal circulation to resume. It interrupts the escalation of tension and pain.
Support your arms
2. Choose seating options that support your arms and spine, like chairs with arm supports, and firm couches with pillows next to you to prop up your arms at your sides. Sitting with arms supported helps diminish the muscle strain, and nervous system tone. This is especially true if you have EDS.
Sit Supported
3. If a chair with arm supports is not available, it is sometimes possible to slide a chair close to a wall, allowing you to gain support from both the wall, and the back of the chair. This works well if you turn the chair sideways so that you are leaning back on the wall and resting one arm on the back of the chair. Ideally, you can switch the position of the back of the chair periodically so that you can support the right and left arm alternatively.
4. Last but not least, sit with your back supported. Put a small pillow or towel at the level of your waist, between your back and the chair. This will lift your chest and put your shoulders and neck in a position that is more efficient at holding your arms. This increased efficiency translates to decreased tension and pain.
Tips 2 – 4 are not as effective as laying on your back with your knees up, 🙂 put they can increase your functional tolerance, slow the onset of pain, and provide some measure of relief in a pinch.
Sources
(www.dysautonomiainternational.org/whatisdys)
Bleasdale-Barr KM and Mathias CJ. Neck and other muscle pains in autonomic failure: their association with orthostatic hypotension. J R Soc Med. 1998;91:355-359.
Water Exercise with EDS: Suggestions for Success
Natalie Dowty, PT, MPT, EdD

The water is an ideal exercise environment for those with chronic pain/illness. The following are a few of the many benefits of the unique properties of water:
- Reduced impact on joints.
- Total body, multi-directional resistance.
- Reduced pain during exercise.
- Support through range of motion.
- Enhanced balance and decreased fear of falling.
- Increased well-being.
In order to make the most of a water exercise program, it helps to be aware specific cautions for those with EDS.
Beware of flotation weights. Most flotation resistance devices are too large and buoyant, and may put unnecessary stress on sensitive joints, especially wrist, shoulder and thumb joints. Attention to hand, wrist and forearm direction against water resistance can get you a great work out without the use of these devices.
Begin your program gradually. Start with 15 minutes or less of water movement and add five or 10 minutes each time, as tolerated. The goal is to avoid aggravating symptoms and to allow connective tissue to adapt to the multidimensional resistance of the water.
Start in chest deep water. Loose joints often respond better in normal standing and walking position, with the feet in contact with the bottom of the pool. This provides stability that deep water exercise does not offer.
Maintain good posture. There’s a tendency to elevate your shoulders when you’re in the water, especially if the water is cool. Try to keep your shoulders down, relax your neck, jaw and back.
Breathe deeply. Along with the tendency to elevate the shoulders, there is a tendency to breathe from the upper chest. The water pressure may make it feel strange, but allow your breath to fill your belly and rib cage in all directions. The water resistance will strengthen your breathing.
Put your heels on the ground. Buoyancy makes us want to stand on and over-use the ball of the foot in the water. Use a heel-toe pattern during water walking to avoid foot pain and so that your heel cords don’t become short and tight.
Move from your core. Use your strong back muscles, rather than your neck, to stabilize your arms. Gently engage your ab muscles before working your arms and legs, to provide a solid center from which to move.
Thin microfiber towels allow you to carry more drying power with less weight.
If you chill easily, here are some additional suggestions:
Wear a close-fitting long sleeve shirt in the water. This holds a layer of warm water next to your skin.
Use a wet shammy (chamois) immediately after leaving the water to remove most of the water from your body and stop evaporation process that cools the skin.
Put on a fleece / microfiber jacket or wrap immediately after exiting the pool. This is particularly helpful if the locker room is cool.

You must be logged in to post a comment.